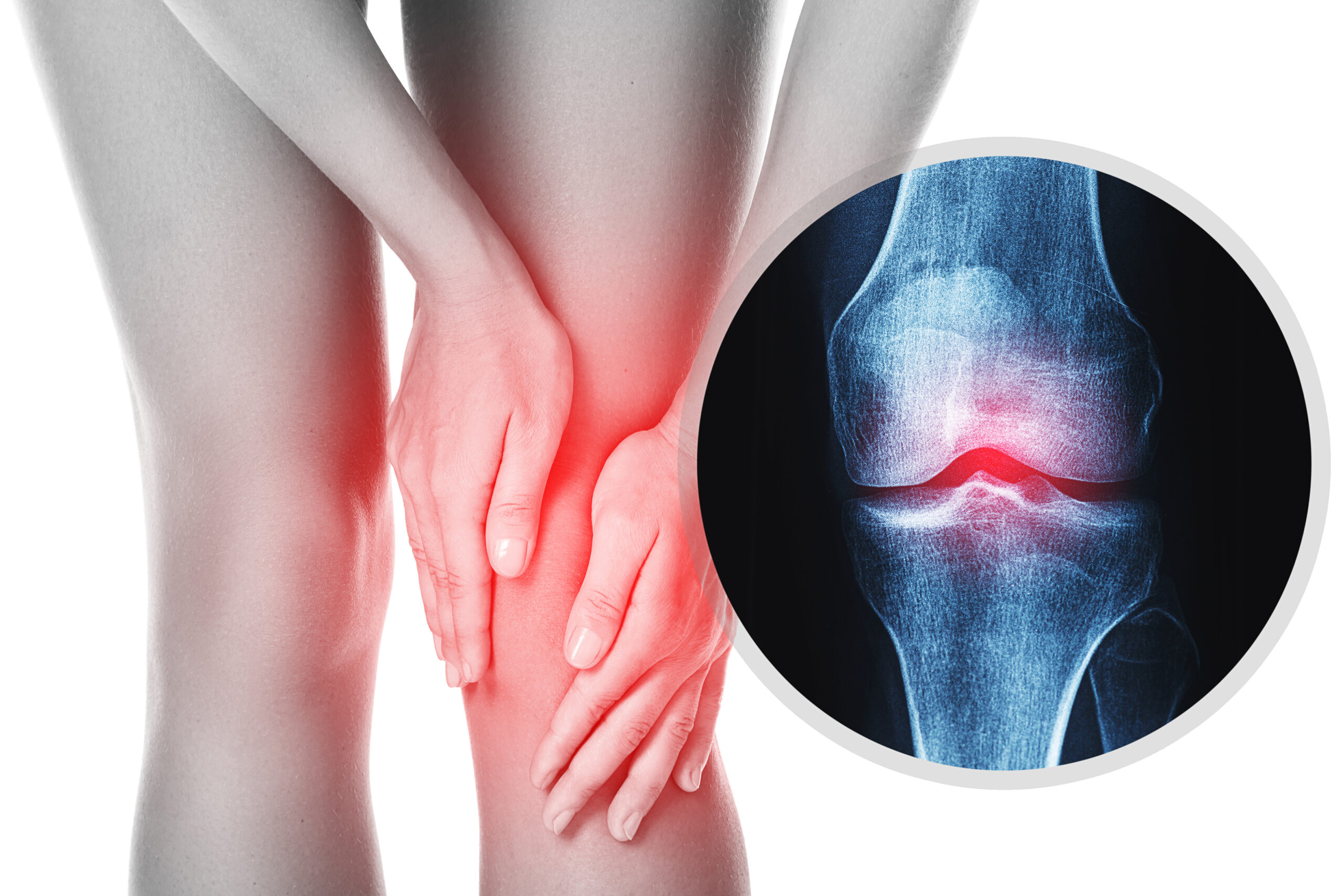
All You Need to Know About Osteoarthritis!
Osteoarthritis (OA) used to be described as an inescapable “wear and tear” condition of the joint for aging adults. However, this is a common misconception! Rather than OA being an inevitable disease, it is actually a degenerative disease of the entire joint that does NOT naturally occur as you age. Some people never develop it! OA is known to be one of the most common forms of arthritis and it can affect any movable joint in your body. OA typically affects the knees, hands, hip, lower back, neck, and big toe. Although there is no cure for OA, there are lots of options to help manage the pain and improve functionality of your joints.
What is Osteoarthritis (OA)?
Before we dive into the condition of OA, let’s explore the anatomy of a typical joint. A joint in your body includes the bone, articular cartilage, lining of the joint – called the “synovium”, and ligaments. The articular cartilage is a layer of cushion-like tissue that is located at the end of your bones; it is responsible for absorbing shock. For example, when you land a jump, the impact of you hitting the ground is very large. The articular cartilages in your joints work to cushion the impact to protect your bones from colliding with each other. The synovium in your joint produces a fluid called the “synovial fluid”. The synovial fluid is a vital component within the joint because it contains all the nutrition and lubrication that you need to maintain a healthy, functional joint.
You might be wondering, what actually causes OA to develop? Unfortunately, there is no one straight answer because OA does not have one single cause. There are many different risk factors that can contribute to the development of the condition:
- Individuals 50+ years of age: OA is typically seen in older individuals, but we also see OA in younger people too!
- Gender: women are more likely to get OA than men.
- Genetic predisposition: if your family members have OA, you are more likely to get it too.
- Previous joint injury: previous injuries to the joint, such as a torn ACL or meniscus, can place you at a higher risk for developing OA in the future.
- Overuse of a joint: this can be in relation to your occupation. Jobs that involve heavy lifting, squatting, kneeling, etc. can contribute to the condition.
- Inactivity: contrary to the prior statement, not moving enough can also put you at risk for developing OA.
- Overweight/obesity: did you know that for weight-bearing joints, such as the knee, each kilogram of extra weight on the joint magnifies the overall weight by up to 7-8 times?
- Muscle weakness: weakness can lead to inadequate support of the joints, which can contribute to the progression of OA.
- Musculoskeletal abnormalities: this may include the malalignment of bones or joint structures.
When small or large injuries happen in regular joints, there is an automatic repair response that works to fix the injury – this includes breaking down areas that were injured (called “degeneration”) and building new parts in replacement (called “regeneration”). In OA, there is an issue with this repair response due to an imbalance of degeneration and regeneration. When OA develops, the articular cartilage can no longer absorb as much impact as it used to, as a result of damage to the articular cartilage and underlying bone. This leads to inflammation (swelling) in the joint and the recruitment of the repair process. However, too much inflammation can lead to a balance disruption between degeneration and regeneration. This means that as the articular cartilage is continually degenerating, the bone is constantly remodelling and building itself back up. Though bone remodelling may seem like a good thing, prolonged and excessive bone regeneration can lead to extra bone growth; these excess bone knobs are called “osteophytes”. The combination of joint inflammation and osteophyte formation may lead to symptoms that you are experiencing, such as pain, stiffness, and loss of normal joint function.
What are common symptoms of Osteoarthritis?
Symptoms of OA typically develop slowly over time and can get progressively worse if not managed properly. Some symptoms may include:
- Pain and/or aching in the joint during activities, after prolonged activity, or at the end of the day
- Pain during activities that load the joint (eg. walking up the stairs, squatting, etc.)
- Joint stiffness in the morning or after prolonged rest that lasts <30 minutes
- Limited joint range of motion
- Limited flexibility
- Clicking, popping, or grating sensation in the joint
- Feeling unstable in the knee or having the knee buckle/give out
- Swelling around the joint
- Weakness in the muscles around the affected joint
It’s important to note that not everyone who has OA experiences pain.
Do I need an X-ray or MRI for Osteoarthritis to be diagnosed?
The answer is no! OA can be clinically diagnosed without the need for diagnostic imaging tools like X-rays or MRIs. Imaging can sometimes be helpful to determine the extent of injury due to the progressive effects of OA. However, it’s important to understand that what is shown on imaging results does not always correlate with the pain you may be experiencing. Some people experience lots of pain from OA, but their imaging results show very little damage. On the other hand, some people may experience very little pain, but their imaging results show large amounts of damage. Physiotherapists will work with you to effectively manage your symptoms based on what your pain levels are, rather than managing your treatment based on imaging results.
What can I do to manage Osteoarthritis?
There are many ways to effectively manage your symptoms when it comes to OA. In fact, one successful method in managing OA is to keep the joint moving! As mentioned earlier, people used to think that OA was a “wear and tear” condition of the joint. This brought on the misconception that if your joint is already getting damaged, you should avoid anything that can cause further damage to it, like moving or using the joint. Contrary to popular belief, we now know that exercise actually plays a HUGE role in decreasing your pain and improving physical function of the joints! But how does moving help the joint? Remember that “synovial fluid” I mentioned earlier? This fluid carries all the nutrients that are vital to the health of the joint. In order for the exchange of nutrients to happen, the joint must move to push the fluid in, out, and around the joint. If there is no movement, the joint cannot absorb the nutrients that it needs to maintain normal joint function and stay healthy. This leads to malnutrition, which further breaks down the structures in the joint – we don’t want this to happen!
Did you know that people with OA experience more falls and are at higher risk of fractures than those without OA? This is because the muscles in the leg get weaker with OA. Without adequate muscle strength to stabilize your legs, you end up more prone to falls and being off-balance. That’s why exercising is even more vital in the management of OA!
A good exercise program to manage OA can be split up into 4 categories:
- Strength training: this can work to increase the strength in your muscles so they can better support the affected joint. It has been shown to decrease pain and increase function of the joint! Strengthening the joint can also work to decrease your risk of falls.
- Aerobic/cardio training: this can work to keep your heart healthy by increasing your stamina and fitness. Fun fact: Nordic walking has been shown in research to have lots of health benefits for those who experience hip OA!
- Neuromuscular training: this category includes components such as sensorimotor (sensation and motor/muscle pathways), proprioception (awareness of your body in space), and balance. It can also include exercises that work on engaging your core and improving your posture, as well as exercises that are more functional to daily tasks.
- Mind/body or stretching exercises: this focuses on increasing your range of motion in the joints to reduce stiffness. People can engage in activities like yoga, Tai Chi, aquatic physiotherapy, and many more!
Make sure you do a 10-minute warm up prior to exercising and a 10-minute cool down after exercising.
Another way to manage OA is through weight management. The body is designed to uphold a certain amount of weight that will not compromise the integrity of the joints. As previously mentioned, extra bodyweight can lead to extra weight on the knee, hip, and ankle joints, which may contribute to your risk of developing OA. By working with physiotherapists and dieticians to develop appropriate weight management strategies, we can take some of that extra pressure off your joints.
Other management options include taking medications to help ease the pain and symptoms you may be experiencing. This can include over-the-counter medications, like Advil or Tylenol, but be sure to talk to your doctor or pharmacist about what options are well-suited for you. Using braces, orthotics, or walking aids may also be helpful to take pressure off your affected joints. The final option is undergoing surgery. Total hip and knee replacements are commonly done to improve pain and function in those with end-stage OA. However, all the non-surgical options mentioned above have been proven to be very effective in managing this condition; therefore, surgery should be considered a last resort.
At Boost Physiotherapy, our physiotherapists are ready to assist you with your injuries and conditions. If you experience any symptoms of OA or would like to learn how to effectively manage your symptoms, be sure to talk to your physiotherapist or physician to determine what treatment options are best suited for your needs. If you have any further questions about OA, book an appointment online or call us today at 587-635-5555 (South Edmonton) or 780-591-5555 (Stony Plain). Our physiotherapists will be happy to assist you in any way!
BY: Laura Schneider
Uncategorized
COMMENTS: No Comments
